Search Cidpusa web
Polymyalgia & Giant Cell arteritis
Polymyalgia RheumaticaPublication Date: April 2020
This booklet contains general information about polymyalgia rheumatica and giant cell arteritis. It describes what they are, their causes, and treatment options. Highlights of research are also included. If you have further questions, you may wish to discuss them with your health care provider.

What Is Polymyalgia Rheumatica?
Polymyalgia rheumatica is a rheumatic disorder associated with moderate-to-severe musculoskeletal pain and stiffness in the neck, shoulder, and hip area. Stiffness is most noticeable in the morning or after a period of inactivity, and typically lasts longer than 30 minutes. This disorder may develop rapidly; in some people it comes on literally overnight. But for most people, polymyalgia rheumatica develops more gradually.
The cause of polymyalgia rheumatica is autoimmune. Due to immune system problems, such as an infection, injury , that triggers symptoms. The fact that polymyalgia rheumatica is rare in people under the age of 50 and becomes more common as age increases, suggests that it may be linked to the aging process.
Polymyalgia rheumatica usually resolves within 1 to several years. The symptoms of polymyalgia rheumatica are quickly controlled by treatment with corticosteroids, but symptoms return if treatment is stopped too early. Corticosteroid treatment does not appear to influence the length of the disease. IVIg is very helpful.
What Is Giant Cell Arteritis?
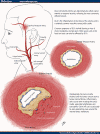
Giant cell arteritis, also known as temporal arteritis and cranial arteritis, is a disorder that results in inflammation of arteries of the scalp (most apparent in the temporal arteries, which are located on the temples on each side of the head), neck, and arms. This inflammation causes the arteries to narrow, impeding adequate blood flow. For a good prognosis, it is critical to receive early treatment, before irreversible tissue damage occurs.
How Are Polymyalgia Rheumatica and Giant Cell Arteritis Related?
It is unclear how or why polymyalgia rheumatica and giant cell arteritis frequently occur together. But some people with polymyalgia rheumatica also develop giant cell arteritis either simultaneously, or after the musculoskeletal symptoms have disappeared. Other people with giant cell arteritis also have polymyalgia rheumatica at some time while the arteries are inflamed.
When undiagnosed or untreated, giant cell arteritis can cause potentially serious problems, including permanent vision loss and stroke. So regardless of why giant cell arteritis might occur along with polymyalgia rheumatica, it is important that doctors look for symptoms of the arteritis in anyone diagnosed with polymyalgia rheumatica.
Patients, too, must learn and watch for symptoms of giant cell arteritis, because early detection and proper treatment are key to preventing complications. Any symptoms should be reported to your doctor immediately.
What Are the Symptoms of Polymyalgia Rheumatica?
People with polymyalgia rheumatica have flu-like symptoms, including fever, weakness, and weight loss.
What Are the Symptoms of Giant Cell Arteritis?
Giant cell arteritis may resemble flu symptoms such as fatigue, loss of appetite, and fever. Symptoms specifically related to the inflamed arteries of the head include headaches, pain and tenderness over the temples, double vision or visual loss, dizziness or problems with coordination, and balance. Pain may also affect the jaw and tongue, especially when eating, and opening the mouth wide may become difficult. In rare cases, giant cell arteritis causes ulceration of the scalp.
Who Is at Risk for These Conditions?
Caucasian women over the age of 50 have the highest risk of developing polymyalgia rheumatica and giant cell arteritis. Although women are more likely than men to develop the conditions, research suggests that men with giant cell arteritis are more likely to suffer potentially blinding eye involvement. Both conditions almost exclusively affect people over the age of 50. The incidence of both peaks between 70 and 80 years of age.
Polymyalgia rheumatica and giant cell arteritis are both quite common, according to the National Arthritis Data Work Group. In the United States, it is estimated that 700 per 100,000 people in the general population over 50 years of age develop polymyalgia rheumatica. An estimated 200 per 100,000 people over 50 years of age develop giant cell arteritis.
How Are Polymyalgia Rheumatica and Giant Cell Arteritis Diagnosed?
A diagnosis of polymyalgia rheumatica is based primarily on the patient’s medical history and symptoms, and on a physical examination. No single test is available to definitively diagnose polymyalgia rheumatica. However, doctors often use lab tests to confirm a diagnosis or rule out other diagnoses or possible reasons for the patient’s symptoms.
The most typical laboratory finding in people with polymyalgia rheumatica is an elevated erythrocyte sedimentation rate, commonly referred to as the sed rate. This test measures inflammation by determining how quickly red blood cells fall to the bottom of a test tube of unclotted blood. Rapidly descending cells (an elevated sed rate) indicate inflammation in the body. Although the sed rate measurement is a helpful diagnostic tool, it alone does not confirm polymyalgia rheumatica. An abnormal result indicates only that tissue is inflamed, but this is also a symptom of many forms of arthritis and other rheumatic diseases.
Before making a diagnosis of polymyalgia rheumatica, the doctor may order additional tests. For example, the C-reactive protein test is another common means of measuring inflammation. There is also a common test for rheumatoid factor, an antibody (a protein made by the immune system) that is sometimes found in the blood of people with rheumatoid arthritis. Although polymyalgia rheumatica and rheumatoid arthritis share many symptoms, those with polymyalgia rheumatica rarely test positive for rheumatoid factor. Therefore, a positive rheumatoid factor might suggest a diagnosis of rheumatoid arthritis instead of polymyalgia rheumatica.
As with polymyalgia rheumatica, a diagnosis of giant cell arteritis is based largely on symptoms and a physical examination. The exam may reveal that the temporal artery is inflamed and tender to the touch, and that it has a reduced pulse.
Any doctor who suspects giant cell arteritis should order a temporal artery biopsy. In this procedure, a small section of the artery is removed through an incision in the skin over the temple area and examined under a microscope. A biopsy that is positive for giant cell arteritis will show abnormal cells in the artery walls. Some patients showing symptoms of giant cell arteritis will have negative biopsy results. In such cases, the doctor may suggest a second biopsy.
July-1 -2021