CIDPUSA.org Autoimmune diseases
Celiac disease: When the body goes against the grain
The celiac iceberg
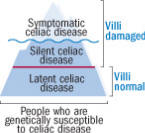
The iceberg represents all people at risk for celiac disease by virtue of their genes. Those with latent celiac disease have no symptoms. Those in the middle have silent or atypical celiac disease -- characterized, for example, by anemia without gastrointestinal symptoms. The proverbial "tip of the iceberg" represents those with the classic symptoms: abdominal bloating, diarrhea, and fatigue, symptoms usually include diarrhea, vomiting, and stunted growth. Older children and adolescents may have stomach pain, canker sores, and tooth enamel defects, and may become depressed or irritable.
Some people diagnosed as adults recall having symptoms during childhood, but many don't. Presumably, they've had latent disease most of their lives, and then something - a viral infection, pregnancy, surgery, or even severe emotional stress --has provoked the symptoms. "Some of my patients tell me that they and their family members all got a viral illness, like the stomach flu. But after the family gets better, their own symptoms never seem to go away,"says Dr. Ciaran Kelly, director of the Celiac Disease Center at Beth Israel Deaconess Medical Center in Boston (BIDMC).
The average age at diagnosis is 46; about 20% of cases are diagnosed after age 60. In addition to anemia and osteoporosis, celiac disease is associated with type 1 diabetes, thyroid problems, and dermatitis herpetiformis, a painful skin condition that involves itchy blisters on the elbows and knees. These associations are strong. For example, the rate of celiac disease in people with type 1 diabetes is four to 10 times the average.
Infertility, recurrent miscarriages, and neurological problems such as ataxia (loss of coordination) have also been linked to this disease.Diagnosis: Blood tests and biopsies
In a person with celiac disease, gluten produces higher-than-normal levels of two antibodies: anti-tissue transglutaminase (tTG-IgA) and antiendomysium (EmA-IgA). The tTG-IgA screening test is the most sensitive; it identifies people who are at risk for celiac disease even if they have no symptoms. If you test positive for these antibodies, Dr. Kelly and other experts strongly recommend that you undergo a small-bowel biopsy to confirm the diagnosis.
(The biopsy is a relatively simple procedure performed under local anesthesia.) Damage to the lining verifies the presence of celiac disease. Knowing for certain is critical because the treatment -- following a gluten-free diet for a lifetime --can be challenging and costly.
Doctors strongly discourage people from trying a gluten-free diet on their own before receiving a firm diagnosis. That's because the antibody tests are accurate only if you are eating gluten-containing foods.
Please continue to Celiac disease testing page