CIDPUSA.org Autoimmune diseases
Whipple's Disease Go to main page of Whipples
Jović NS, Jović JZ.
Department of Neurology and Psychiatry for Children and Youth, University Medical School, Belgrade.
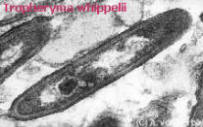
The disease is named after George H. Whipple who, in 1907, was the first to describe an intestinal "lipodystrophy". Although Whipple's disease is generally recognized as a multisystem chronic granulomatous disease, primarily involving the digestive system, it can also appear as a primary neurological disorder in rare cases. Most often it is manifested with loss of weight, diarrhea, malabsorption, abdominal pain, lymphadenopathy, cardiopathy, hyperpigmentation and hypotension. The presence of periodic acid-Schiff (PAS)-positive macrophages in biopsy specimens (not only jejunal) and demonstration of "Whipple's bacilli" visible by electron microscopy, are diagnostic signs of active Whipple's disease.
Whipple's disease confined to the CNS is rare. It is rarely found in the differential diagnosis of patients with progressive neurological deterioration. The most common neurological picture includes progressive dementia, external ophalmoplegia, myoclonus, seizures, ataxia, hypothalamic dysfunction (sleep disorders, hyperphagia, polydipsia) and meningitis. Oculofacial-skeletal myorhythmia as a movement disorder, associated with Whipple's disease, is reported. Fulminant course of cerebral Whipple's disease is unusual and unfavourable. The confusing and nonspecific clinical appearance is typical for primary CNS involvement. It has recently been suggested that CNS involvement occurs in all cases, although only 10-20% of patients may show it. The CNS is the most common site of disease relapse. The CT scans and MRI of the brain are often normal, but may show cortical/subcortical atrophy, hydrocephalus, focal or intracerebral mass lesions. The cerebrospinal fluid can sometimes contain PAS-positive macrophages. Brain biopsy is suggested as a diagnostic method in cases of high suspicion of CNS Whipple's disease. However, the lesions are frequently inaccessible and false negative. Without extended antibiotic therapy, the course of Whipple's disease is lethal. Now, the prognosis is good, although the optimal antimicrobial regimen is not clearly established. Initial parenteral therapy (tetracycline, penicilline, streptomycine, chloramphenicol, ampicilline) and peroral long-term treatment with trimetoprime-sulphametoxasole, are recommended. As CNS relapse of Whipple's disease may occur after several years, long-term treatment should include antibiotics that are able to cross the blood-brain barrier. The CNS relapse, in contrast to the systemic ones, is resistant to the treatment. Appropriate therapy instituted earlier in the course of the disease is associated with a better neurological outcome. Early recognition can be critical in Whipple's disease because of irreversible neurological sequelae seen later in the course of this potentially treatable condition. In cases with high clinical suspicion in which Whipple's disease cannot be diagnosed with procedures such as jejunal biopsy, antibiotic therapy is recommended. Recovery of an established neurological deficit may rarely occur. Longterm follow-up studies would help to identify the optimal antibiotic regimen and duration of treatment.
.
What are the signs and symptoms of Whipple's disease?
Signs and symptoms of Whipple's disease vary widely.
Classic signs and symptoms of Whipple's disease
include
periodic joint pain, with or without inflammation, that may persist for years before the appearance of other symptoms
chronic diarrhea, with or without blood
weight loss
abdominal pain and
bloating
fever
fatigue
anemia a condition in which the blood has a lower-than-normal number of red blood cells
Less common signs and symptoms of Whipple's disease include
darkening of the skin
enlarged
lymph nodes
chronic cough
chest pain
pericarditis inflammation of the membrane surrounding the heart
heart failure
Neurologic symptoms occur in some people diagnosed with Whipple's disease and can mimic
symptoms of almost any other neurologic condition.
Neurologic symptoms of Whipple's disease include
Vision problems
Dementia
Facial numbness
Headache
Muscle weakness or twitching
difficulty
walking
Memory problems
Strokes
Dysautonomia
OpthalomplegiaSymptoms of neurologic, lung, or heart disease occasionally appear without gastrointestinal symptoms.
Continue to the treatment of Whipples